Blood clots are your body's way of stopping bleeding, but sometimes they form where you don't want them. A clot in a deep leg vein (deep vein thrombosis, DVT) can break off and travel to the lungs (pulmonary embolism, PE) — that’s dangerous. This page explains how clots form, who’s at risk, what to watch for, and simple steps to lower your risk.
Clotting usually happens when one or more of three things go wrong: the vein wall is damaged, blood flow slows down, or your blood gets stickier than normal. You’ll hear this called Virchow’s triad, but you don’t need fancy words to act on it. Common triggers are long flights or car rides, being immobile after surgery, injury to a vein, pregnancy, certain cancers, and some medications like estrogen-containing birth control or hormone replacement pills.
Other risk factors include age (risk rises after 60), obesity, smoking, family history of clots, and active inflammation or infection. If you have a recent operation or long anesthesia, your risk goes up because you’re lying still and your veins aren’t pumping blood back to the heart well.
Prevention is practical and works. If you’re traveling, get up and walk every hour, do ankle pumps and calf raises in your seat, and stay hydrated. After surgery, follow your care team’s plan: use compression stockings, wear sequential compression devices if prescribed, and try to walk as soon as it's safe. If you’ve had a clot before or have a strong risk, your doctor may prescribe blood thinners like heparin, warfarin, or direct oral anticoagulants (apixaban, rivaroxaban).
Know the warning signs. For a DVT in the leg: swelling (often one leg), pain or tenderness, warmth, and redness. For a PE: sudden shortness of breath, sharp chest pain that may worsen with breathing, fast heartbeat, lightheadedness, or coughing up blood. Any of those symptoms deserve urgent attention — call emergency services or go to the ER.
Doctors diagnose clots with tests like a duplex ultrasound for legs, a D-dimer blood test to check clot breakdown products, and CT pulmonary angiography for suspected PE. Treatment usually starts with anticoagulants to stop the clot growing. Severe cases may need clot-busting drugs or procedures, and very rarely an IVC filter to catch clots before they reach the lungs.
Small steps add up: move regularly, avoid long immobility when possible, maintain a healthy weight, quit smoking, and tell your doctor about any family history of clots. If you’re about to have surgery or plan a long trip and have risk factors, talk with your healthcare provider about extra precautions. Quick action and simple prevention can make a big difference.
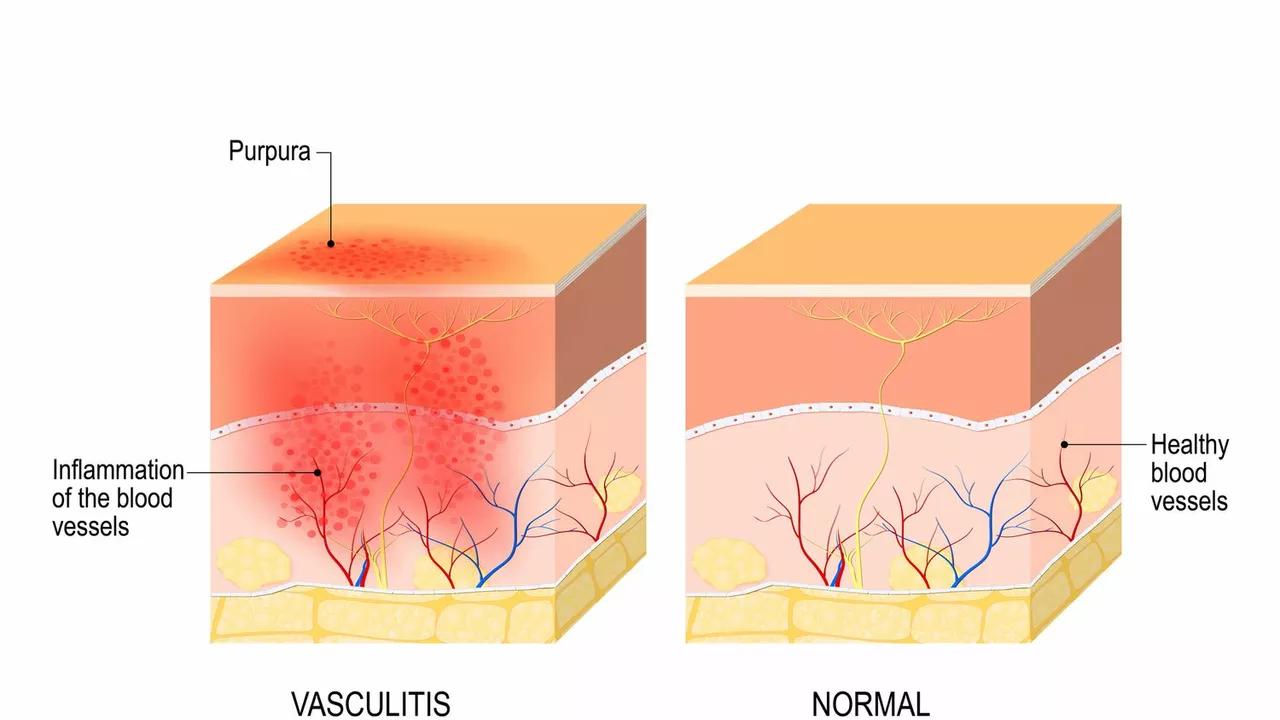
Hey there folks! Let’s dive into an entertaining yet essential health topic - the fascinating link between inflammation and blood clot formation (sounds like a thrilling blockbuster, right?). It's like a dynamic duo, but instead of fighting crime, they're potentially causing health issues. Recent studies show that inflammation is like a sneaky little ringleader, triggering our body to produce more blood clots. These clots are like overzealous party guests, sometimes creating chaos (read: blockages) in our blood vessels. So, take care of your body, folks - it's the only place we have to live, after all!
READ